Please, don’t say “all kids do that,” because even if behaviors look the same, that doesn’t mean they are the same for our kids from hard places.
The impact of trauma on the developing brain
The potential effects of trauma and abuse on the developing brain and nervous system are powerful and incredibly complex.
Healthy brain development is highly contingent upon a number of highly interrelated neuroregulatory systems that are highly sensitive to the effects of environment and experience. In some instances, environmental factors influence the expression of genes responsible for proteins affecting neurotransmitter sensitivity and function. In other instances, circulating hormones affect development of critical brain regions associated with learning, memory, impulse control, mood and emotional self-regulation.
The neuroregulatory systems that help us to manage stress throughout life are extremely malleable during the prenatal period and early childhood. Toxic levels of stress during this period affect the development of these neuroregulatory systems in ways that cause those systems to become overly responsive to shut down in response to a wide range of stressors in later life.
Let’s look at how toxic stress affects the development of different systems and structures in the brain…
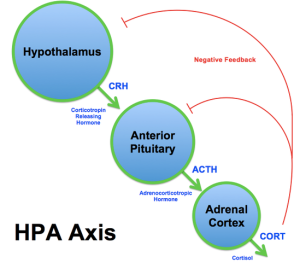
The hypothalamic-pituitary axis (HPA): The HPA plays a critical role in the body’s response to stress. The hypothalamus produces corticotropin-releasing hormone (CRH) which stimulates the pituitary gland to produce adrenocorticotropic hormone (ACTH). ACTH acts on the adrenal gland to increase levels of cortisol (see diagram at top of page). Cortisol is a steroid hormone produced in response to a wide variety of stressors. Cortisol mobilizes energy stores and suppresses immune response. Surgeons prefer to operate early in the morning when cortisol levels tend to be at their highest. Long-term elevation of cortisol levels in children (as seen in kids exposed to high levels of acute or chronic stress/abuse) can turn off the glucocorticoid receptor gene (involved with regulation of the long-term stress response of the brain to cortisol) and the myelin basic protein gene, producing the “insulation” of nerve cells that allows for efficient nerve signal transmission. Elevated cortisol levels also cause damage to the hippocampus (below).
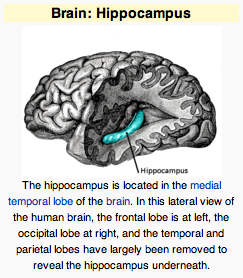
The hippocampus: The hippocampus is a structure that plays a key role in learning by consolidating information from short-term to long-term memory. The hippocampus is capable of growing new neurons in adulthood. Damage to the hippocampus from elevated cortisol levels in childhood leads to impairments in learning and memory.
The locus coeruleus/noradrenergic brain systems: The locus coeruleus is a region located in the brainstem where the cell bodies of most noradrenergic neurons are located. This system is involved with regulating the overall level of arousal in the central nervous system. Exposure to stress/trauma early in life have been associated with lifelong increases in noradrenergic reactivity.
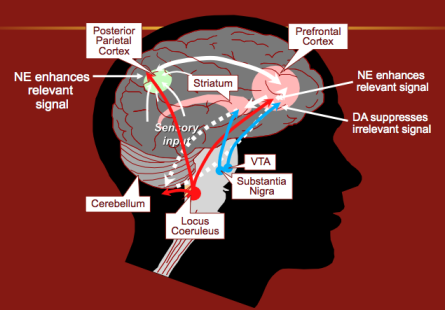
The noradrenergic system (along with the dopaminergic system) is the primary system associated with executive functioning. Tracts of neurons originating in the locus coeruleus project to the posterior attention center in the parietal cortex (responsible for scanning the environment for relevant stimuli) and the anterior fronto-striatal system, which is more involved with executive control and focusing attention. The posterior center is primarily under noradrenergic control, while the anterior center receives both dopaminergic and noradrenergic projections. Difficulties associated with weaknesses in executive functioning include poor impulse control, diminished capacity for emotional self-regulation, delaying gratification and problems with working memory. Editor’s note: This may help to explain the increased prevalence of ADHD among kids who have been traumatized or abused along with the observation they are frequently less responsive to medication than kids with ADHD lacking such exposure.
Dopaminergic systems: Numbing, decreased interest in pleasurable activities and difficulties with ability to maintain focus upon a task are associated with pathways mediated by dopamine. Dopamine pathways originating in the midbrain projecting to the medial prefrontal cortex may be especially vulnerable to the effects of acute and chronic stress. These pathways also play a role in selective information processing, working memory, and applying previously learned information to new experiences. Pathways from the medial prefrontal cortex to the amygdala are thought to play a role in mediating the response to fear.
Serotonergic/GABA systems: Alterations in these systems in response to stress/trauma contribute to difficultiess in social attachment and regulation of mood and affect following early stress.
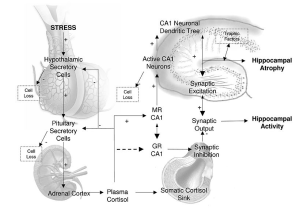
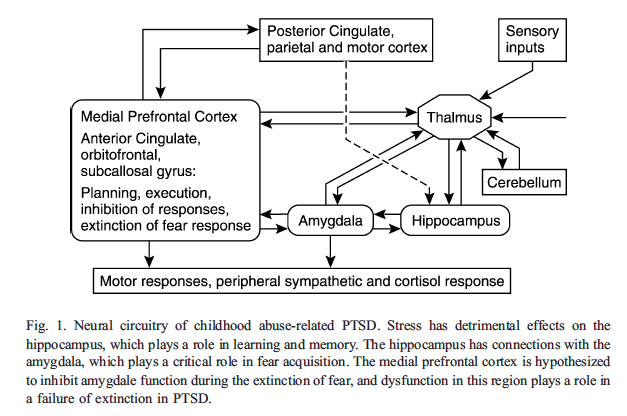
Here’s a diagram from an article in Child and Adolescent Psychiatric Clinics of North America that shows the interrelationship of the different neural circuits involved in childhood PTSD…
Bottom line…The neuroendocrine changes that occur in response to trauma in children are widespread, long-lasting, and impact mood, learning, arousal, impulse control, memory, emotional self-regulation, and contribute greatly to future response to stress.
Updated March 4, 2016
Disinhibited Social Engagement Disorder… The new term for Reactive Attachment Disorder?
We’ll take a closer look in this post at the new companion diagnosis to Reactive Attachment Disorder related to pathologic care in early childhood… Disinhibited Social Engagement Disorder.
Studies of children who have been maltreated or raised in institutions have demonstrated two characteristic patterns of emotional response and behavior in response to pathologic caregiving environments. The first pattern involves emotional withdrawal…kids who lacked a preferred attachment figure, failed to respond to comfort when distressed, demonstrated decreased social and emotional reciprocity, decreased positive affect and unexplained fearfulness or irritability. Their symptoms could be described as internalized. This is the group we discussed in a previous post who will continue to be described as meeting criteria for Reactive Attachment Disorder (RAD). In contrast, the second group was observed to demonstrate indiscriminately social behavior-inappropriately approaching unfamiliar adults and a lack of concern for strangers… in some instances, a willingness to wander away with strangers. They may also exhibit a lack of ability to maintain an appropriate sense of body space, and may also demonstrate disinhibition of behavior.
Research has demonstrated that these two patterns differ in terms of clinical correlates, course, and response to treatment. There was also much greater interrater reliability among clinicians using diagnostic criteria based upon the assumption that the two patterns represented separate and distinct conditions compared to the existing DSM-IV criteria for Reactive Attachment Disorder. As a result, the authors of the DSM-5 chose to establish a separate diagnosis of Disinhibited Social Engagement Disorder (DSED) to distinguish the second group from children with Reactive Attachment Disorder. This new designation corresponds to the condition in the ICD-10 referred to as Disinhibited Attachment Disorder of Childhood. Disinhibited Social Engagement Disorder encompasses the vast majority of children and teens we’ve treated in our practice who in the past were identified with attachment disorders.
Here are the criteria for Disinhibited Social Engagement Disorder in the DSM-5:
A. A pattern of behavior in which a child actively approaches and interacts with unfamiliar adults and exhibits at least two of the following:
- Reduced or absent reticence in approaching and interacting with unfamiliar adults.
- Overly familiar verbal or physical behavior (that is not consistent with culturally sanctioned and with age-appropriate social boundaries).
- Diminished or absent checking back with adult caregiver after venturing away, even in unfamiliar settings.
- Willingness to go off with an unfamiliar adult with little or no hesitation.
B. The behaviors in Criterion A are not limited to impulsivity (as in Attention-Deficit/Hyperactivity Disorder) but include socially disinhibited behavior.
C. The child has exhibited a pattern of extremes of insufficient care as evidenced by at least one of the following:
- Social neglect or deprivation in the form of persistent lack of having basic emotional needs for comfort, stimulation and affection met by caregiving adults.
- Repeated changes of primary caregivers that limit ability to form stable attachments (e.g., frequent changes in foster care).
- Rearing in unusual settings that severely limit opportunities to form selective attachments (e.g., institutions with high child to caregiver ratios).
D. The care in Criterion C is presumed to be responsible for the disturbed behavior in Criterion A (e.g., the disturbances in Criterion A began following the pathogenic care in Criterion C).
E. The child has a developmental age of at least nine months.
Specify if Persistent: The disorder has been present for more than 12 months.
Specify current severity: Disinhibited Social Engagement Disorder is specified as severe when a child exhibits all symptoms of the disorder, with each symptom manifesting at relatively high levels.
First, we’ll start by looking at the similarities between kids with DSED and RAD. Both conditions are linked to social deprivation, neglect and pathologic care, and are readily identified among children being raised in institutional settings. Both conditions appear to be relatively stable over time in institutionalized children. But some very key differences exist as well…
- Some kids continue to exhibit symptoms associated with DSED after establishing selective or secure attachments with adoptive or foster parents, while RAD has only been observed in research studies among children who lack attachments.
- DSED appears not to be responsive (or only minimally responsive) to enhanced caregiving, whereas RAD is often very responsive. One study done in Romania comparing foster care to institutionalized care found a significant reduction in signs of RAD among children placed in foster care, but no reduction in the signs of DSED.
- Kids with DSED are often interested in, and willing to interact with unfamiliar adults, while kids with RAD typically demonstrate limited interest in interaction with unfamiliar adults.
- Kids with DSED appear to be at greater risk of developing externalizing disorders (ADHD, Oppositional Defiant Disorder, Conduct Disorder) whereas kids with RAD are more vulnerable to internalizing disorders (depressed mood).
- Kids described with DSED are prone to social and verbal intrusiveness and attention-seeking behavior during childhood, and superficial peer relationships along with enhanced peer conflicts during adolescence. The presentation of RAD in childhood and adolescence is less clear.
- Kids with DSED are more likely to be confused with kids with ADHD, while kids with RAD are more likely to be confused with kids with autism. Lack of capacity for self-regulation in social situations is a key feature of DSED, while a lack of comfort-seeking behavior is characteristic of DSED.
We can anticipate lots of confusion because the vast majority of children presenting for clinical care will meet the diagnostic criteria for DSED as opposed to RAD, since DSED is more likely to persist after kids leave pathologic care and causes more difficulties with interpersonal relationships. DSED is easier to observe across settings, especially in schools. I can certainly understand why the name of the condition was changed…not all kids with DSED lack attachments…but I’m not sure this distinction will be recognized by a majority of clinicians for quite some time.
Updated March 1, 2016